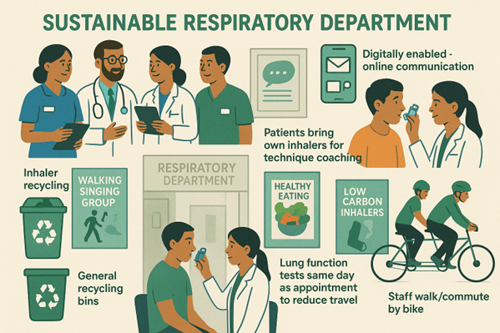
Sustainability should be built into the way organisations deliver care, not added on afterwards. Respiratory teams can influence change by linking projects to Green Plans, patient care, and cost savings.
Governance and Strategy
- Make sure your Trust or ICB has a Net Zero lead, board group and Green Plan in line with NHS guidance.
- Push for sustainability to be part of business cases and service changes (triple bottom line: clinical, financial, environmental).
- Link respiratory work with Core20PLUS5 priorities to address inequality.
Procurement and Prescribing
- Work with procurement teams on supplier standards (e.g. Evergreen assessment).
- Ensure formularies support low-carbon inhalers and devices where clinically appropriate.
- Review use of consumables and equipment — avoid single-use where safe alternatives exist.
Services and Estates
- Ask if your organisation has a climate adaptation plan (heatwaves, extreme weather, medicine storage).
- Strengthen digital/remote services to cut unnecessary travel while keeping care accessible.
- Check facilities support active travel and provide green spaces and healthy food.
Culture and Communication
- Join existing sustainability groups or QI teams — build on what’s already happening.
- Share progress through short updates and celebrate small wins.
- Link with external networks to spread ideas and gain support.
If you want to go fast, go alone. If you want to go far, go together.
Before starting from scratch, see if you can build on existing work.
Check if your organisation or ICB already has:
- A Green Plan or sustainability strategy
- A sustainability lead or committee (if yes, consider joining!)
- Ongoing QI work you could contribute to (e.g. see the QI section for examples eg inhaler recycling or telehealth expansion)
Share Your Progress and Impact once you get started
- Use short updates to share what’s happening (emails, posters, newsletters, update slides at meetings)
- Celebrate small wins—even basic changes like switching to digital patient info leaflets or adding air pollution advice to asthma action plans
- Use your results to get further support or expand your work
- Measure impact in as many useful ways as possible
Connect to Broader Networks for Support
- You’re not alone! Joining a professional network can help you find ideas, collaborators, and encouragement.
If you’re embarking on a new project your first action should be to map out who you will need to speak to and include.
Depending on the scale and scope of the project these may include:
| Internal |
External |
- Colleagues in your department
- Clinical leads
- Other departments (eg adult/Paeds, ED)
- Pharmacy
- Nursing teams
- Estates and facilities staff
- Lung function physiologists
- Sustainability officers
- Procurement team
- Admin and management teams
- Finance teams
- Communications team
|
- council officers
- Public health teams
- Smoking cessation services
- Regional networks
- Community organisations
- Patient representatives/groups
- Integrated Care Board staff
|
It can be useful to think in advance about barriers you may face, so that you don’t hit a wall early on, and you are ready with a constructive response to any challenges.